If you were undergoing a surgical procedure, would you ever think to refuse the antibiotics your physician had ordered to prevent an infection?
For most hospitalized patients, that would be unfathomable. And yet, when it comes to another common complication with a far greater death toll than surgical-site infections, both patients and health care professionals aren't nearly as vigilant. Each year, dangerous blood clots claim the lives of about 100,000 Americans. Many of those deaths occurred during or after a hospitalization, despite evidence showing that most of these events could have been prevented.
The most dangerous clots are those that travel to the lungs, a potentially fatal event known as pulmonary embolism that makes it difficult or impossible to breathe. Clots can also form in large veins in the leg — a condition called deep vein thrombosis — where they cause pain and swelling. These clots can become pulmonary embolisms when they break off and travel toward the lungs.
Hospitalized patients face a higher risk of these scary complications, which also go by the acronyms PE and DVT. During periods of hospitalization, conditions are ripe for clot formation. When we experience trauma, whether it's due to an auto accident or going under the surgical knife, there is a larger chance of a blood clot breaking off. (Indeed, former NBA star Jerome Kersey died this year from a pulmonary embolism following knee surgery.) Patients with cancer, heart disease and lung disease, and obese patients, pregnant women and those who have just delivered a baby also have elevated risks of harmful clots.
Still, blood clots are under the radar. Most of these cases are preventable when patients are screened for their risk of clot formation and are provided therapy to match that risk. Yet many patients do not receive appropriate therapy.
Before The Johns Hopkins Hospital focused on this several years ago, physicians prescribed risk-appropriate therapies approximately half of the time — mirroring the performance of many other hospitals. Then an improvement team made a host of changes, such as creating a "hard stop" in our computerized ordering system that made it mandatory for physicians to review blood clot prevention. Now, we prescribe appropriate therapies for more than 96 percent of patients, and blood clots have gone down.
It's tempting to chalk up the remaining clots to the patient's condition — their cancer, surgery or just plain bad luck — yet we kept looking for ways to further prevent these complications. And we soon learned that measuring how often a doctor prescribes a therapy doesn't always equal how often a patient receives that therapy.
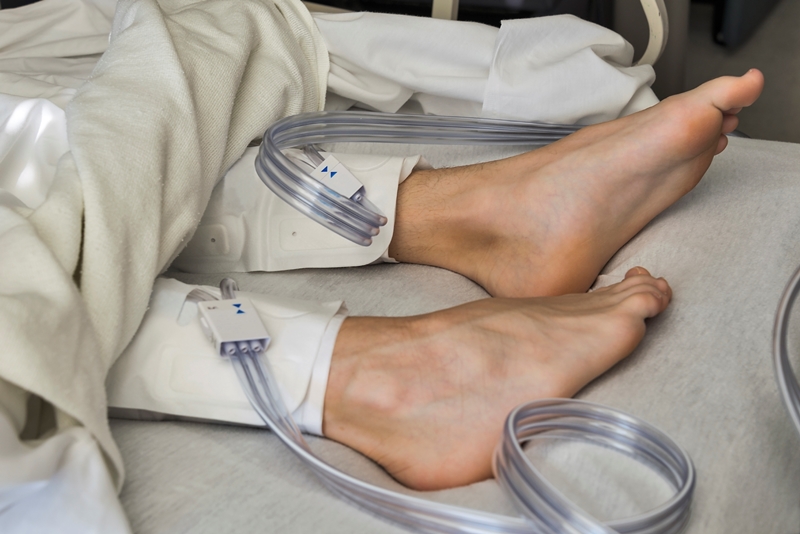
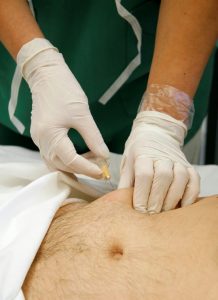 Studies by our hospital’s researchers showed that nearly 12 percent of the physician-prescribed doses of blood clot prophylaxis never reach patients. About 60 percent of those missed doses were due to patient refusal. Some don’t want the injections of anti-clotting medication, which is typically delivered via a needle in the belly. Others don’t understand the reason they are supposed to wear the "squeezy boots" or other mechanical devices that keep blood moving in legs and feet.
Studies by our hospital’s researchers showed that nearly 12 percent of the physician-prescribed doses of blood clot prophylaxis never reach patients. About 60 percent of those missed doses were due to patient refusal. Some don’t want the injections of anti-clotting medication, which is typically delivered via a needle in the belly. Others don’t understand the reason they are supposed to wear the "squeezy boots" or other mechanical devices that keep blood moving in legs and feet.
Researchers also found that nurses' attitudes regarding blood clot prevention played a role in missed doses. They sometimes second-guessed physicians' orders and presented the preventive steps as optional when speaking to patients. Some nurses believed that if patients were walking, they didn't need to worry about clots — a stance not supported by the scientific evidence. Yet in one study conducted on hospital floors, researchers heard statements such as: "Hey, Mr. R, it's time for your heparin dose, but as long as I see you up, high-fiving me in the hallways, we can hold off for now."
Elliott Haut, a Johns Hopkins trauma surgeon on our blood clot prevention team, says that focusing on missed doses has the potential to be a "game changer," helping us realize dramatic reductions in this complication. Missing even a single dose of heparin, a common anti-clotting medication, increases your risk of developing a blood clot. Respecting patient preferences is important for clinicians, but both they and patients should be fully aware of these risks.
Perhaps one reason that blood clots do not get enough attention is that they often strike after a patient has gone home. In seconds, you can go from feeling normal to struggling for air, with a sharp pain in your chest as clots block the main arteries to your lungs. The clinicians who took care of you in the hospital probably don’t know if you are readmitted or — worse — pass away from preventable blood clots.
All of us — physicians, nurses, patients and their families — need to work together and do a better job of raising the profile of this danger. The needless suffering is real and largely expensive. Yet change occurs not only by directing the mind, but by motivating the heart and removing barriers to better care. As such, with funding from the Patient-Centered Outcomes Research Institute, we recently worked with blood clot survivors to develop an educational video and handout for patients about prevention. It has been said that statistics are humans with the tears wiped away. The stories in the videos put back those tears and hopefully will encourage everyone to take an active role in preventing these complications.
Learn More:
- Preventing Venous Thromboembolism: Johns Hopkins Armstrong Institute for Patient Safety and Quality
- ClotCare
- National Blood Clot Alliance
- North American Thrombosis Forum
This post first appeared on the U.S. News and World Report Patient Advice blog.
Another amazing article from Dr. Pronovost.
Suggested related reading:
A) "Reality check for checklists"
http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(09)61440-9/fu
B) The Checklist Paradox – Lorelei Lingard – video:
https://vimeo.com/78557791
C) book "Safe Patients, Smart Hospitals"
D) book "Unaccountable: What Hospitals Won't Tell You and How Transparency Can Revolutionize Health Care"
https://www.youtube.com/watch?v=dTeKiNP_Y64
A cut whether big or small should never be taken lightly. A small disfigure such as a blood clot could somehow cause major disease if not treated well. Always took on consideration those little details. Practicing better work ethics and analysing the patient's state before release should always be number one priority.
Pingback: Blood Clots: The Least-Appreciated Complication of Hospital Care? | Doctella
A small scar should also be taken seriously as no care can result into a blood clot which if not treated well can cause a big problem. Thanks for sharing such a blog.
This is a really great post! Thanks so much for sharing!
always i used to read smaller posts which also clear their
motive, and that is also happening with this paragraph which I am
reading here.
Hello! I just want to give you a big thumbs up for
the great information you have got right here on this post.
I'll be returning to your site for more soon.
Hello! Someone in my Facebook group shared this website with us so I came
to give it a look. I'm definitely enjoying the information. I'm book-marking and will be
tweeting this to my followers! Terrific blog and fantastic design and style.
Heya! I just wanted to ask if you ever have any trouble with hackers?
My last blog (wordpress) was hacked and
I ended up losing a few months of hard work due to no
back up. Do you have any methods to protect against hackers?
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://accounts.binance.com/register?ref=P9L9FQKY
Spot on with this write-up, I really believe this website needs a lot more attention. I'll probably be returning to read through more,
thanks for the info!
Hi there to every single one, it's genuinely a nice for me to pay a visit
this web page, it contains priceless Information.
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
Sweet blog! I found it while surfing around on Yahoo News.
Do you have any tips on how to get listed in Yahoo News?
I've been trying for a while but I never seem to get there!
Appreciate it
I am curious to find out what blog platform you have been using?
I'm experiencing some minor security issues with my latest site and
I'd like to find something more risk-free. Do you have any solutions?
Hi, just wanted to say, I loved this post. It was helpful.
Keep on posting!
Stunning quest there. What happened after? Good luck!
Hello There. I found your blog using msn. This is a very well written article.
I will make sure to bookmark it and return to read more of
your helpful information. Thanks for the post. I'll certainly comeback.
I know this if off topic but I'm looking into starting my own blog
and was wondering what all is required to get setup? I'm assuming having a blog like yours would cost a pretty penny?
I'm not very web savvy so I'm not 100% positive.
Any recommendations or advice would be greatly appreciated.
Thanks
My coder is trying to convince me to move to .net from
PHP. I have always disliked the idea because of
the costs. But he's tryiong none the less. I've been using Movable-type on several websites for about a year and am concerned about switching to another platform.
I have heard fantastic things about blogengine.net.
Is there a way I can transfer all my wordpress content
into it? Any help would be really appreciated!
Hi there! Do you know if they make any plugins to
assist with SEO? I'm trying to get my blog to rank for some targeted keywords but I'm not seeing
very good gains. If you know of any please share. Appreciate it!
Hi, for all time i used to check website posts here early in the dawn, since
i love to learn more and more.
Hi there, just became alert to your blog through Google, and found that it's truly
informative. I'm gonna watch out for brussels.
I'll appreciate if you continue this in future. Lots of people will be benefited from your writing.
Cheers!
whoah this weblog is magnificent i love studying your posts.
Stay up the great work! You already know, many individuals are hunting round for
this information, you can help them greatly.
Thank you for sharing your thoughts. I truly appreciate your efforts and
I am waiting for your further write ups thank you once again.
Saved as a favorite, I love your blog!
Hey very nice blog!! Man .. Excellent .. Wonderful ..
I will bookmark your blog and take the feeds also? I'm glad to seek out numerous helpful information right
here in the publish, we need develop extra strategies on this regard, thank you for sharing.
. . . . .
What's Taking place i am new to this, I stumbled
upon this I've discovered It absolutely useful and it has aided me out loads.
I'm hoping to contribute & assist other customers like its aided me.
Good job.
It's really very difficult in this busy life to listen news on Television, thus I simply use web for that reason, and take the hottest information.
What a data of un-ambiguity and preserveness of precious experience on the topic
of unpredicted emotions.
Asking questions are really nice thing if you are not understanding anything entirely, except this paragraph
gives nice understanding yet.
What's Taking place i am new to this, I stumbled upon this I've
found It absolutely helpful and it has helped me out loads.
I'm hoping to give a contribution & assist other users
like its helped me. Good job.
It's going to be ending of mine day, but before ending I
am reading this wonderful post to increase my know-how.
Pretty! This was an incredibly wonderful post.
Many thanks for providing this info.
This article is both informative and inspiring. The real-life examples were my favorite part. This was worth reading from start to finish.
always i used to read smaller content that as well
clear their motive, and that is also happening with this
piece of writing which I am reading here.
Thank you for your shening. I am worried that I lack creative ideas. It is your enticle that makes me full of hope. Thank you. But, I have a question, can you help me?
Your style is unique in comparison to other folks I've read stuff from.
Thanks for posting when you've got the opportunity,
Guess I will just bookmark this web site.
Hey there! I realize this is sort of off-topic however I needed to ask.
Does building a well-established blog like yours take
a large amount of work? I'm brand new to blogging however I
do write in my journal daily. I'd like to start a blog so I
will be able to share my personal experience and views online.
Please let me know if you have any suggestions or tips for new aspiring bloggers.
Thankyou!
Just desire to say your article is as astounding. The clarity for your submit is
just cool and that i can suppose you are an expert in this subject.
Well with your permission allow me to clutch your feed to keep updated
with approaching post. Thank you one million and please keep up the gratifying
work.
I have read so many articles or reviews on the topic of the blogger lovers however this post
is truly a nice piece of writing, keep it up.
Wonderful, what a blog it is! This website gives valuable data to us, keep it up.
I'm impressed, I have to admit. Rarely do I come across
a blog that's both equally educative and
amusing, and without a doubt, you've hit the nail on the head.
The problem is something too few folks are speaking intelligently
about. I'm very happy that I came across this during my hunt for something concerning this.
Simply wish to say your article is as surprising.
The clarity in your post is just excellent and i could assume you're an expert on this subject.
Well with your permission allow me to grab your feed to
keep updated with forthcoming post. Thanks a million and please
carry on the enjoyable work.
Great post, you have pointed out some wonderful details , I also conceive this s a very fantastic website.
Wow that was unusual. I just wrote an really long comment but after
I clicked submit my comment didn't show up. Grrrr... well I'm not writing
all that over again. Anyways, just wanted to say great
blog!
Hi, I think your blog might be having browser compatibility issues.
When I look at your blog in Safari, it looks fine but when opening in Internet Explorer, it
has some overlapping. I just wanted to give you a quick heads up!
Other then that, wonderful blog!
Hmm is anyone else encountering problems with the
pictures on this blog loading? I'm trying to find out if its a problem on my end or if it's the blog.
Any feedback would be greatly appreciated.
Remarkable issues here. I'm very satisfied to
see your post. Thank you so much and I am taking a look forward to contact you.
Will you please drop me a e-mail?
all the time i used to read smaller posts that as well clear their
motive, and that is also happening with this post
which I am reading at this time.
Hi there, I discovered your blog by way of Google
whilst searching for a comparable topic, your site came up,
it appears to be like good. I've bookmarked it in my google bookmarks.
Hi there, just became aware of your weblog via Google, and located that it's truly informative.
I am gonna watch out for brussels. I will appreciate for those who continue this in future.
Many other people will likely be benefited out of your
writing. Cheers!
This is very interesting, You're a very skilled blogger. I have joined your feed and
look forward to seeking more of your great post. Also, I've shared your site in my social networks!
I feel that is one of the so much significant info for me.
And i'm happy studying your article. However should commentary on few common issues, The
web site taste is ideal, the articles is actually excellent
: D. Just right activity, cheers
You are so awesome! I do not believe I have read something like that before.
So wonderful to find someone with a few original
thoughts on this topic. Seriously.. many thanks for starting
this up. This website is something that's needed on the internet,
someone with a bit of originality!
This design is steller! You obviously know how to keep a reader amused.
Between your wit and your videos, I was almost moved to start my own blog (well, almost...HaHa!) Wonderful job.
I really loved what you had to say, and more than that, how you
presented it. Too cool!
Awesome post.
I know this if off topic but I'm looking into
starting my own blog and was curious what all is needed to get set up?
I'm assuming having a blog like yours would cost a pretty penny?
I'm not very internet smart so I'm not 100% positive.
Any tips or advice would be greatly appreciated. Cheers
What's up it's me, I am also visiting this site on a
regular basis, this website is truly pleasant and the viewers are really sharing fastidious thoughts.
Wow, this article is good, my younger sister is analyzing such
things, so I am going to convey her.
Paragraph writing is also a excitement, if you be familiar
with afterward you can write otherwise it is difficult to write.
Hey! I know this is kinda off topic but I was wondering which
blog platform are you using for this website?
I'm getting tired of WordPress because I've had problems with hackers and I'm looking at options for another platform.
I would be awesome if you could point me in the
direction of a good platform.
It's a pity you don't have a donate button! I'd certainly donate to this superb blog!
I suppose for now i'll settle for bookmarking
and adding your RSS feed to my Google account. I look forward to new updates and will talk about this blog with my Facebook group.
Talk soon!
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.info/register?ref=P9L9FQKY