In 2013, a 52-year-old man went to an emergency department complaining of dizziness. Physicians evaluated him, decided that it was a benign condition — as it usually is — and sent him home. Days later, it became apparent that this was no harmless event. He suffered a significant stroke, with permanent disability as the result. He's now out of work and can't drive.
As it turns out, his 53-year-old brother went to a different ED one month later with the same symptoms. But this time, when a physician told him his dizziness was not serious, his family remembered his brother's misfortune and urged them to take a closer look. They identified a stroke early, treated him and avoided any disability.
These brothers, who reached out to me after hearing of my research into missed strokes in the ED, are emblematic of the challenges that we face in eliminating misdiagnosis in medicine. When we think of diagnostic errors, our minds might gravitate to cases such as radiology studies that are misread or unread, letting a cancer go unnoticed and untreated. In truth, such events represent a small piece of the total misdiagnosis burden. Much more prevalent are those cases in clinics and EDs in which a commonplace symptom can have an uncommon cause. Dizziness and vertigo, for example, are responsible for 4.4 million ED visits each year in the U.S. Typically, the symptoms result from an inner ear infection or other relatively minor cause, but in 3 to 5 percent of those cases, the patient is having a stroke. And of these strokes, roughly 35 percent are misdiagnosed.
This dynamic puts these cases in a problematic "sweet spot": The symptom happens much too frequently for each patient to see a specialist, and yet the danger is significant enough that front-line physicians must still investigate.
Other symptoms have similar dynamics. We miss the uncommon (yet not rare) aneurysms in people with headaches, sepsis in patients with fever and pulmonary emboli in people with shortness of breath.
The mission of reducing misdiagnosis may sound a little quixotic at first. Of course, we cannot end human error. However, when we view this challenge from a public health perspective, we can focus on categories of diagnosis that affect large populations of patients. And for several of these common complaints, there is hope that we can do a much better job of finding those with the potential to be harmful or fatal.
A Model System: Improving Stroke Diagnosis
When a patient presents in the ED complaining of dizziness or vertigo, the doctor might order a radiology exam to reach a diagnosis. However, head CT scans — often used for patients with dizziness — miss 80 to 90 percent of early-onset strokes in these patients. MRI scans do better but still miss between 10 and 20 percent of strokes in the first 48 hours after symptoms begin.
There is one diagnostic approach that catches nearly all strokes in these patients — a series of eye-movement tests that evaluate what is known as the eye-ear balance reflex. Highly trained specialists can tell, based on slight variations in eye movements, whether vertigo is due to a benign inner ear condition or a stroke.
Unfortunately, only about 500 physicians in the world have this skill set, which can take several years of training to acquire.
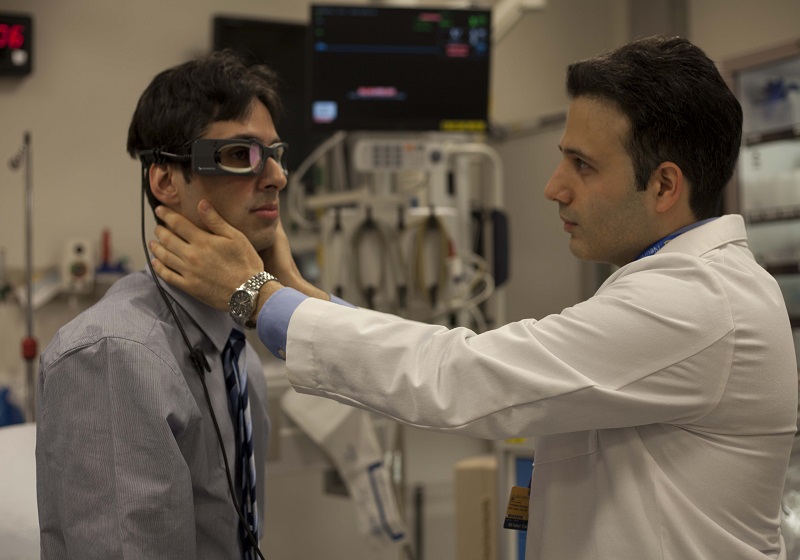
Technology may help us bridge the gap, translating this evidence to hospitals everywhere. A video-oculography machine, including a set of goggles outfitted with a small video camera, can detect the minute eye movements that few physicians can distinguish and interpret. In a small test of 20 patients, we found the device-based approach to be 100 percent accurate at discerning strokes from benign ear conditions. Now, we are undertaking a randomized clinical trial to evaluate this solution's effectiveness in the ED when paired with computer-based decision support.
Promising Research
This is a microcosm for how one might investigate a type of misdiagnosis. First, we identify and describe the problem, understanding the standard of care and current diagnostic practices. Second, we find methods to improve diagnostic accuracy. Finally, we seek to translate that knowledge from the bedside to the population, whether it's through a simple paper tool or advanced technology.
Other exciting research is taking a similar approach, with the promise of improving diagnosis of dangerous conditions that often lurk behind common ailments.
- Subarachnoid hemorrhage. When patients present to the ED with severe headaches, it can be hard to pick out those with a serious condition. As a result, about 5 percent of these patients with confirmed subarachnoid hemorrhages are initially misdiagnosed during their initial ED visit. In Ottawa, Canada, emergency medicine physician Jeffrey Perry and colleagues have developed bedside clinical decision rules to help "rule out" hemorrhages in low-risk patients while identifying those who need further examination. In a study involving 10 EDs, their rules would have identified 260 of 262 patients who had hemorrhages, and reduced by 10 percent the use of CT scans and lumbar punctures, which are used to confirm these hemorrhages.
- Brain swelling. Patients with headaches, changes in vision and neurologic deficits may have a serious condition, such as a stroke, brain tumor or blocked flow of spinal fluid. Physicians can use the ophthalmoscope to examine the back of the eyes for evidence of high pressure in the head or other signs of neurologic injury, but this is an underutilized, imperfect and time-consuming process, requiring the eyes to be dilated. So Emory University neuro-ophthalmologist Beau Bruce and colleagues found a new approach. Using a special camera, a nurse takes pictures of the back of patients' eyes — without needing to dilate them — and sends the images to Bruce's team for review. They found that 13 percent of patients screened with this device had important missed eye findings that changed the diagnosis and that this method easily detected dangerous conditions that were otherwise overlooked. Snapping the photos is simpler than taking someone's blood pressure.
- Heart attacks. Standard diagnostic tests for heart attack look for traces of a biomarker protein called troponin. Yet this test often fails to identify these events in women. A new, higher-sensitivity troponin test can identify twice as many heart attacks in women, University of Edinburgh researchers reported in 2015. As lab and imaging tests advance, our diagnostic accuracy will improve.
A Path Forward
Taking on diagnostic errors can seem overwhelming, but we don't have to look far for a model of how to address such a big problem. Roughly a decade ago, we began to see how health care-associated infections could be reduced by going after them one category at a time, rather than by taking a blanket approach. Starting with central line-associated bloodstream infections, Johns Hopkins experts summarized the evidence into checklists and other tools, coupling that with culture change to alter provider behaviors. These infections were cut drastically in Michigan, then nationwide and in other countries. Health care has since turned its attention to other infections, using similar approaches but with different evidence, checklists and tools.
I believe we can drastically reduce diagnostic errors in much the same way: creating a model for success and taking on one piece at a time, rather than treating it as a monolithic problem. In my opinion, missed stroke in acute dizziness and vertigo is a critical exemplar that will lead our charge toward stamping out harms from diagnostic error across a broad range of conditions.
Learn about the new Armstrong Institute Center for Diagnostic Excellence.
Misdiagnosis Facts
- Misdiagnosis may account for 40,000 to 80,000 preventable deaths annually in U.S. hospitals.
- 12 million Americans are misdiagnosed each year in ambulatory care; up to one-third of them may suffer serious harm.
- Roughly 10 percent of all strokes are not recognized upon initial medical contact.
- As many as 165,000 cerebrovascular events, such as strokes and hemorrhages, are misdiagnosed in U.S. Emergency Departments each year. More than half of these cases are dismissed as benign dizziness or headaches.
Free webinar: "Diagnosis as a Team Sport"
Join David Newman-Toker from 1-2 p.m. EST on March 1, 2017 for a discussion how physicians can use teamwork — with patients, family members and other health care professionals — to improve diagnostic accuracy. Details and registration.
Pingback: Common Symptoms, Uncommon Causes: Reducing Misdiagnosis on the Front Lines | Health Jobs Nationwide
I really believe in misdiagnosis. I was first diagnosed with viral encephalitis in 1997. I've been falling and having coordination problems. I tore my acl, had back surgery and foot surgery. I've been still falling, I've been told it's hallucination, bipolar, and depression. The doctors have been giving me nasid, antidepressants and stating, beta blockers and it's always in my mind. My digestive disease doctor told me from all the meds I was given it have elevated ammonia levels. Now I have 5 extra veins in my liver and had to have 5 shunts. My legs have been swelling and I continue to tell the doctors and going to the er and it's always the same. I just fell at a store last month and it still I'm crazy. My new cardiologist said my vein going to my heart completely. This week I'm having an angioplasty and I'm so scared because I have almost died 3 times and was in I currently 4 times. I was put in restraints because of meds I was given and was allergic to. Only one nurse told me something I never heard a medical professional say because I did work in a hospital before she told me all the problems you are going through is because the meds you are getting you are having an allergic reaction to. And on all my records they are changing dates when a new diagnosis started. In 2014 is when they found out I had liver disease my general practice doctor put 2011 and I have the records. My new cardiologist has that I seen her in 2015 and I first saw her in 2016 and I have all the records and charts. After I went to the er last month and they said I was hallucinating and all my test was normal five days later the doctor calls me and says I have a uti. We as patients have to pray because doctors are only human but even though you make a mistake you don't have to lie and make the patient feel like they don't know their own bodies.
Pingback: Diagnostic Errors are a Problem!
Excellent article and this is one of the reasons we started out company 🙂 Too many folks get unnecessary tests and medicine for vertigo--and vice versa. We created affordable infrared goggles and a training program focused on point-of-contact clinicians to help make this an effective triage tool. I hope we can work together to eliminate this all too common problem!
They are amazing and Useful to all people. Thanks for sharing this post and Impressive site.